So, let’s talk about that heavy feeling we sometimes get. You know, like when everything just seems gray? That’s major clinical depression sneaking in.
It’s not just about feeling sad. It’s like this cloud that follows you around, no matter how hard you try to shake it off. Honestly, it can feel overwhelming.
Imagine waking up and feeling like getting out of bed is a monumental task. Or maybe you used to love hanging with friends, but now you’d rather stay home scrolling through your phone. Yeah, it can be rough.
The thing is, understanding depression in a psychological context helps us see it’s not just «in your head.» There are complex factors at play—biology, life events, and thoughts that all mix together.
So I thought we should break this down together! Let’s explore what major clinical depression really is and how it fits into our lives.
Understanding the Differences Between Major Depressive Disorder and Clinical Depression
Major Depressive Disorder (MDD) and Clinical Depression often get tossed around as if they’re the same thing. But, there’s a bit of nuance here. Let’s break this down, shall we?
First off, **Major Depressive Disorder** is a specific diagnosis in the realm of mental health. It’s characterized by several symptoms that impact your daily life. You might feel persistent sadness, lose interest in things you once loved, or struggle with sleep. And it’s not just a passing mood; these feelings can last for weeks or even months.
On the other hand, when people talk about **Clinical Depression**, they’re usually referring to Major Depressive Disorder in a broader sense. This term can sometimes include other forms of depression too. It essentially means that the depression is serious enough to require professional treatment.
Now let’s get into some key differences:
- **Symptoms**: MDD has a defined set of symptoms that must be present for at least two weeks for diagnosis. Think fatigue, feelings of worthlessness, and difficulty concentrating.
- **Duration**: In MDD, symptoms last most of the day, nearly every day. Clinical Depression shares this but may encompass various depressive disorders over time.
- **Types**: MDD is one type of clinical depression, but there are others like Dysthymia (persistent depressive disorder) or Seasonal Affective Disorder (SAD), which may affect individuals differently throughout seasons.
- **Severity**: The term “clinical” usually implies severity and consistency that disrupt normal functioning across different areas of life—work, relationships, etc.
Now think about someone named Sarah. She used to love hiking but finds herself avoiding it lately because she feels empty and unmotivated. She might have MDD if this has been going on for over two weeks straight. If her doctor says she has clinical depression instead? That could mean she might have experienced similar episodes before or that her current state is part of a larger pattern.
So remember, while all Major Depressive Disorders fall under the umbrella of Clinical Depression— not all clinical depression equals MDD specifically! Does that clear things up a bit? It’s understandable why folks confuse them; mental health language can be tricky.
When approaching treatment options or understanding how these conditions affect someone’s life, distinguishing between them helps tailor the right support needed for healing and recovery!
Understanding the Four Key Causes of Depression: Insights and Implications
Depression is one of those things that can feel like a heavy fog. It creeps in silently and wraps around you, making everything seem dull and gray. But it’s not just one thing causing it. There are four key causes we can look at to better understand major clinical depression.
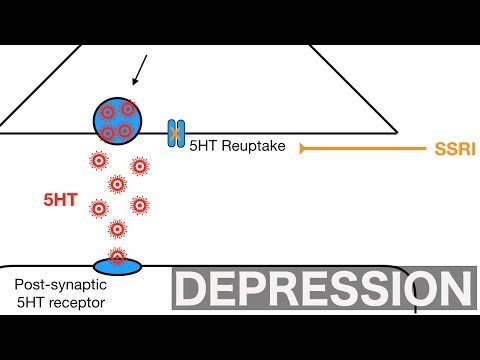
- Biological Factors: Your brain chemistry plays a huge role. Neurotransmitters like serotonin and dopamine are responsible for mood regulation. If these chemicals are out of balance, you might feel down more often or intensely. Think about someone who’s been prescribed antidepressants—these meds often target those chemical imbalances to help restore a sense of normalcy.
- Genetic Predisposition: Depression can run in families, which means if someone close to you has experienced it, your chances might increase too. It’s like inheriting traits, only with emotional well-being instead of curly hair or blue eyes. You know, if your mom had severe depression, that could mean you’re more likely to experience something similar.
- Environmental Stressors: Life events can really affect mental health—stressful situations like job loss, relationship breakdowns, or losing a loved one often trigger depression. So picture this: you just got laid off from a job you loved; the loss and uncertainty could lead to feelings of sadness and hopelessness.
- Psycho-social Factors: This one is all about how you think and interact with others. Negative thought patterns can trap you in cycles of despair. Maybe you’ve noticed that when you’re feeling low, your inner critic gets louder—telling you things like you’ll never be happy again or no one cares about you.
While these factors are distinct, they don’t exist in isolation; they all intertwine in complex ways. For example, having a genetic predisposition doesn’t guarantee you’ll develop depression—it needs that environmental push sometimes.
You know how some days feel heavier than others? Well, understanding these causes helps us see why some people might sink deeper into the fog while others manage better with similar struggles.
Managing depression isn’t straightforward since every person’s experience is unique. But understanding these four key factors gives us better insights into *how* we can approach it—not just for ourselves but for our friends too! So if you or someone close feels that gray creeping in more often than usual, knowing what’s behind those feelings can make a real difference in seeking help or support.
Understanding Major Depressive Disorder in DSM-5: Criteria, Diagnosis, and Implications
Major Depressive Disorder (MDD), often just called depression, is more than just feeling sad. It’s a serious mental health condition that affects millions of people around the world. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) outlines specific criteria for diagnosing this disorder. You can’t really diagnose it based on just a bad day or two; there’s a whole list of symptoms to consider.
So, what are those criteria? Basically, to be diagnosed with MDD, you need to experience at least five of the following symptoms during the same two-week period:
- Depressed mood: Feeling sad or empty most of the day, nearly every day.
- Anhedonia: Losing interest or pleasure in activities you once enjoyed.
- Significant weight change: Gaining or losing weight without trying.
- Sleep disturbances: Experiencing insomnia or sleeping too much.
- Fatigue: Feeling tired or lacking energy almost all the time.
- Feelings of worthlessness: Having excessive guilt or self-blame.
- Difficulties in concentration: Struggling to focus on tasks that were once easy for you.
- Recurrent thoughts of death: This includes not just fear of dying but thinking about suicide as well.
Now, let’s talk about the idea behind these criteria. They’re designed to capture how depression can impact your emotional state and daily life. Imagine going through a time when you used to love hanging out with friends but now can barely get out of bed—that’s serious stuff!
The thing is, it’s not just about checking off those boxes. A healthcare professional considers how these symptoms affect your functioning in different areas—like work and relationships. That’s crucial because sometimes people might look fine on the outside but feel awful inside.
Diagnosis isn’t solely based on symptoms either. It also involves ruling out other medical conditions that could be causing similar feelings or behaviors. For example, thyroid issues can create depressive-like symptoms too! So yeah, a doctor would want to make sure they have the full picture.
Implications of an MDD diagnosis are pretty significant. For one thing, it can help you get access to treatments tailored specifically for you—like therapy or medication if needed. But there’s also stigma surrounding mental health disorders that might weigh heavy on some folks’ minds. It’s really important for society as a whole to recognize that mental health should be treated with as much urgency and care as physical health.
In short, understanding Major Depressive Disorder through the lens of DSM-5 helps in recognizing its complexity and severity—you follow me? It’s not just another label; it’s an opportunity for healing and understanding oneself better amidst life’s ups and downs.
Major clinical depression is a heavy topic, and it can be hard to wrap your head around. You might know someone who has gone through it, or maybe you’ve faced those dark clouds yourself. It’s not just feeling sad for a day or two; it goes way deeper than that. Seriously, this isn’t just a “bad day for you;” it’s more like a bad season that seems never-ending.
Think about this: imagine waking up one morning and just feeling like you’re carrying the weight of the world on your shoulders. Even getting out of bed feels like climbing a mountain. That’s what major depression can do—it can zap your energy and motivation, making everything feel pointless or overwhelming. You could have people around you telling you how great life is, but it’s like you’re in a different universe where you can’t seem to find joy in anything.
There are also some really important psychological components at play here. When someone is experiencing major depression, it often affects how they think about themselves and their world. Negative thoughts can swirl around like a storm—you know, thoughts like “I’m worthless” or “I’ll never be happy again.” It’s easy to get caught in that cycle where each negative thought leads to another. The worst part? It’s hard for people on the outside to see these internal battles.
Take my friend Lily, for instance. She was always the life of the party—funny, smart, and outgoing. Then one day, she just started pulling away from everyone for no clear reason. At first, we all thought she was just busy with work or something like that. But in reality? She was fighting this invisible monster called depression that made her feel trapped even when she was surrounded by friends who loved her.
On the flip side, what’s striking about major clinical depression is how it can look different from person to person. Some folks might sleep all day while others can’t sleep at all; some might lose interest in things they used to love while others may feel irritable and restless instead of sad.
It’s also quite common for people dealing with major depression to experience physical symptoms as well—things like fatigue, headaches, or aches that don’t seem to have an obvious cause. That connection between mind and body is fascinating yet frustrating because it’s layered—the emotional pain often shows up as physical discomfort.
Having open conversations about mental health helps chisel away at the stigma surrounding conditions like major clinical depression. Talking about how you’re feeling—even if it’s tough—can make all the difference.
Depression isn’t anyone’s fault; it’s complex and influenced by everything from genetics to life experiences and social support systems (or lack thereof). Knowing more about its psychological context doesn’t give answers overnight but helps us build empathy for those who are wrestling with these feelings.
So yeah, understanding major clinical depression isn’t easy but being supportive and compassionate toward ourselves and others goes a long way in helping lift those heavy clouds bit by bit.


